Sunlight, Skin, and Balance
A clinical perspective on exposure, oxidative stress, and resilience
Sunlight is not inherently harmful.
It regulates circadian rhythm, influences cortisol and melatonin cycles, supports nitric oxide release, and enables cutaneous vitamin D synthesis. Human biology evolved in relationship with light.
But ultraviolet radiation is biologically active energy. When UV photons penetrate the skin, they interact with DNA, proteins, and lipids — initiating measurable biochemical responses.
The conversation around sun exposure is often polarized. The physiology is not.
Understanding UV Radiation
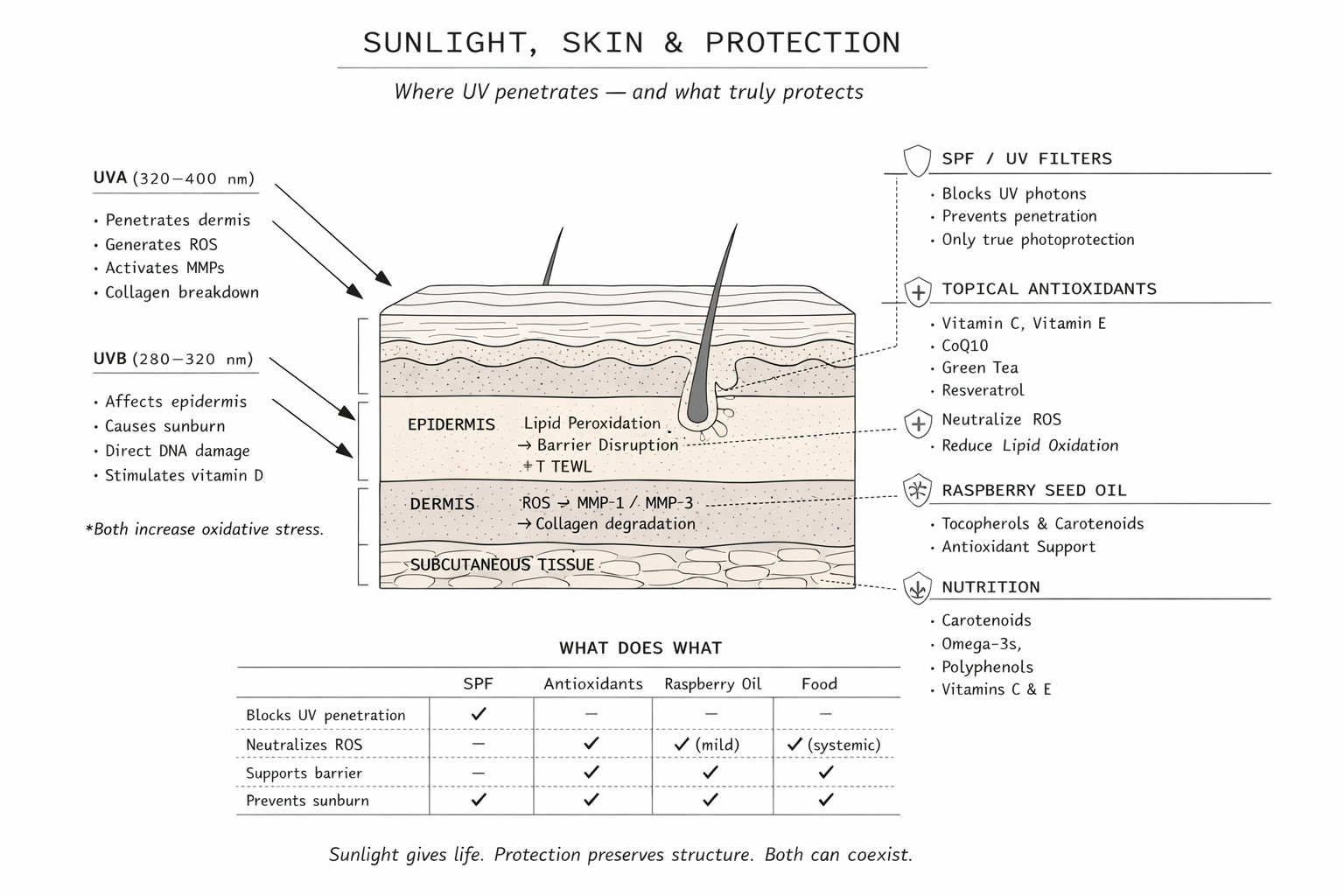
Two primary forms of ultraviolet light reach the earth’s surface:
UVA (320–400 nm)
Penetrates into the dermis, generates reactive oxygen species (ROS), contributes significantly to photoaging, and passes through clouds and glass.
UVB (280–320 nm)
Primarily affects the epidermis, causes erythema (sunburn), directly damages DNA through pyrimidine dimer formation, and drives vitamin D synthesis.
Both increase oxidative stress. The difference lies in depth and mechanism.
Oxidative Stress and Structural Change
UV exposure increases formation of reactive oxygen species such as superoxide anion, hydrogen peroxide, and hydroxyl radicals. These molecules oxidize cellular lipids, proteins, and nucleic acids.
In the dermis, ROS activate matrix metalloproteinases (MMP-1 and MMP-3), enzymes that degrade collagen and extracellular matrix proteins. Over time, this contributes to structural thinning and loss of elasticity.
In the epidermis, UV exposure disrupts keratinocyte differentiation and increases lipid peroxidation, weakening the intercellular lipid matrix composed of ceramides, cholesterol, and free fatty acids. This destabilizes barrier function and increases transepidermal water loss (TEWL).
The skin does repair itself — through DNA repair enzymes, melanin production, and endogenous antioxidants like glutathione and superoxide dismutase. But cumulative exposure gradually outpaces repair.
Protection moderates this load.
Where Antioxidants Truly Fit
Topical antioxidants neutralize reactive oxygen species by donating electrons before oxidative chain reactions propagate.
Clinically relevant examples include:
L-ascorbic acid (vitamin C)
Tocopherol (vitamin E)
Ferulic acid
Coenzyme Q10
Green tea catechins
Resveratrol
Carotenoids
These reduce lipid peroxidation, stabilize membranes, and may downregulate MMP activation.
And raspberry seed oil?
Raspberry seed oil contains tocopherols and carotenoids, offering antioxidant support. It contributes to reducing oxidative stress within the lipid environment of the skin.
However, claims of meaningful natural SPF are overstated. While it may exhibit minor UV-absorbing properties in laboratory conditions, it does not provide reliable, standardized photoprotection.
It is best understood as an antioxidant-supportive lipid — not a substitute for UV filters.
Antioxidants mitigate downstream damage.
They do not prevent UV penetration.
Internal Photoprotection and Nutrition
Diet influences systemic antioxidant capacity and inflammatory response.
Carotenoids accumulate in the skin over time and may modestly increase resistance to UV-induced erythema.
Examples of supportive foods include:
Carotenoids:
Carrots, sweet potatoes, spinach, kale, red bell peppers, tomatoes, watermelon
Vitamin C:
Citrus, strawberries, kiwi, guava
Vitamin E:
Almonds, sunflower seeds, hazelnuts
Polyphenols:
Green tea, cacao, blueberries, pomegranate
Omega-3 fatty acids:
Wild salmon, sardines, chia seeds, flax seeds
These nutrients enhance resilience. They do not create an internal SPF. Their effects are cumulative and supportive — not protective in isolation.
Barrier Integrity and Tolerance
A stable stratum corneum improves recovery capacity.
The outer layer of the skin functions as a brick-and-mortar system: corneocytes embedded within a lipid matrix of ceramides, cholesterol, and free fatty acids. UV-induced lipid peroxidation can destabilize this structure.
When the barrier is intact, inflammatory signaling is moderated and repair is more efficient.
Protection is not only about filters. It is also about maintaining structural integrity.
When Awareness Matters Most
Certain ingredients increase photosensitivity:
Retinoids
Alpha hydroxy acids
Beta hydroxy acids
Benzoyl peroxide
Essential oils containing furanocoumarins (e.g., bergamot, cold-pressed citrus)
With these, UV exposure has amplified effects. Intelligent protection becomes more important — not from fear, but from physiology.
A Balanced Perspective
I do not advocate for complete sun avoidance.
Morning light regulates the nervous system. Moderate exposure supports systemic health. The relationship with sunlight should not be rooted in anxiety.
But from a dermatologic standpoint, repeated high-intensity, unprotected exposure accelerates oxidative damage and structural breakdown over time.
The goal is informed exposure.
Support the barrier.
Use antioxidants strategically.
Nourish internally.
Choose protection that is wearable and sustainable.
Closing
Skin health is cumulative biology.
Every day of light exposure contributes to a long-term equation — not in a dramatic, immediate way, but gradually, quietly, over decades.
Sunlight gives life.
Protection preserves structure.
Both can coexist without contradiction.
The work is not to eliminate light.
It is to understand how light interacts with the skin — and to respond with intelligence rather than fear.
Balance is not passive.
It is intentional.